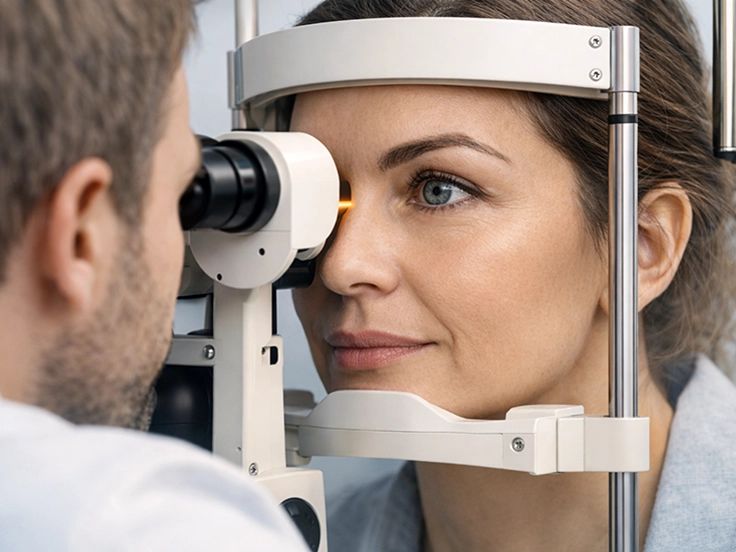
If your eyes feel dry, irritated, or watery, your tear film may not be working the way it should. Dry eye can affect both daily comfort and clear, stable vision, especially with screen time or contact lenses. At Peak Vision Care in Newton, MA, we offer dry eye evaluations and treatment plans tailored to your symptoms and tear film needs.
During your visit, Dr. Denis Shlosman will evaluate your symptoms and use advanced dry eye imaging to assess tear meniscus height, non-invasive tear breakup time, meibomian glands, and ocular surface fluorescein staining patterns to identify what’s driving your discomfort and which treatments are most likely to be effective.
We offer dry eye treatment options including:
- Step-by-step home care routine - from drops and lid hygiene to prescription options
- In-office treatments for dry eye and meibomian gland dysfunction (MGD)
- Advanced in-office options: IPL, Low Level Light Therapy (LLLT), and OptiVize
Understanding Dry Eye (Ocular Surface Disease)
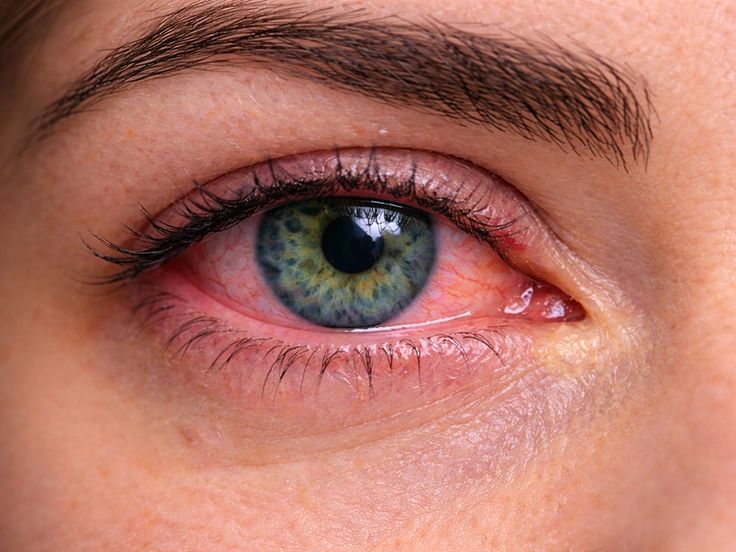
Dry eye happens when your tear film is not doing its job - either you are not making enough tears, or your tears evaporate too quickly. For many people, the issue is evaporative dry eye, which is often linked to the meibomian glands in your eyelids. These glands produce oils that help keep tears from drying out too fast. When the glands are blocked or not working well, your eyes can feel irritated even if they water.
Dry eye can be influenced by aging, certain medications, and systemic conditions such as Sjögren’s syndrome, rheumatoid arthritis (RA), and lupus. Treating dry eye matters because symptoms can worsen over time, and in severe cases, ongoing dryness can irritate and damage the surface of the eye.
Common dry eye symptoms
- Dryness or tightness
- Burning or stinging
- Gritty or sandy feeling
- Redness and irritation
- Watery eyes (reflex tearing)
- Fluctuating or blurry vision, especially with screens or contact lenses
Dry eye causes

- Meibomian gland dysfunction (MGD) - oil glands in the eyelids get blocked or underproduce oil, so tears evaporate too quickly.
- Not making enough tears - tear production can decrease with age or certain health conditions.
- Aging - natural changes in tear production and eyelid glands can make dryness more common over time.
- Medications - some prescription and over-the-counter meds can contribute to dryness (your doctor can review your list).
- Autoimmune / systemic conditions - conditions like Sjögren’s syndrome, rheumatoid arthritis (RA), and lupus can affect tear production and the ocular surface.
- Screen time and reduced blinking - staring at screens can reduce blink rate and lead to faster tear evaporation.
- Contact lens wear - contacts can disrupt the tear film and worsen dryness for some patients.
- Environmental factors - wind, smoke, dry indoor heat, and air conditioning can dry out the tear film.
- Eyelid inflammation (blepharitis) - irritation at the eyelid margin can affect tear quality and gland function.
- Hormonal changes - can influence tear production and dry eye symptoms.
Your Dry Eye Evaluation
- Symptom review + lifestyle triggers (screens, contacts, environment)
- Eyelid + meibomian gland assessment
- Tear film testing (TBUT, staining, etc. as applicable)
Dry Eye Treatment Options

Daily at-home care - Foundational routines that support comfort and tear stability, such as lubricating drops, warm compresses, and eyelid hygiene.
Prescription support - Targeted therapies to reduce inflammation, improve tear quality, and help break the cycle of irritation when home care is not enough.
Advanced in-office therapies - In-office treatments designed to address meibomian gland dysfunction and evaporative dry eye, including IPL, Low Level Light Therapy (LLLT), and OptiVize.
Severe / regenerative options - For more advanced cases, specialized therapies like autologous serum tears and amniotic membranes to support the ocular surface.
Advanced in-office dry eye therapies
These in-office treatments are designed to target the underlying causes of dry eye, especially meibomian gland dysfunction (MGD). They can help improve the quality of the tear film, reduce irritation, and support longer-lasting comfort. Most patients find these treatments easy to tolerate with little to no downtime.
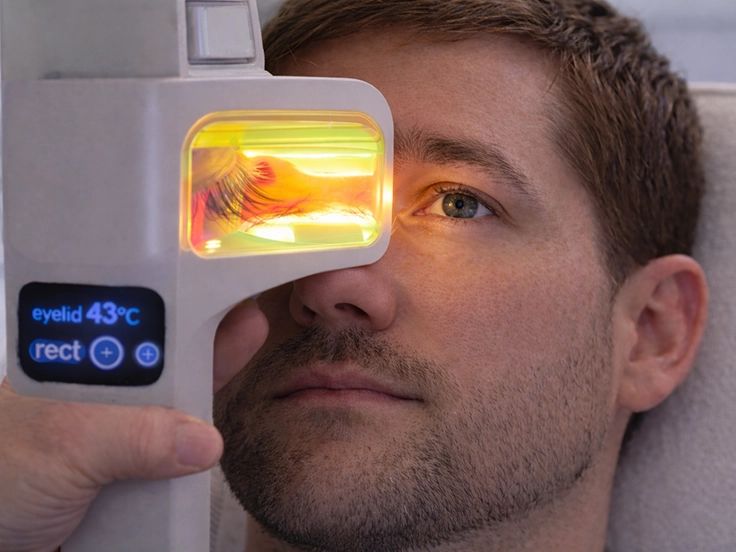
IPL (Intense Pulsed Light)
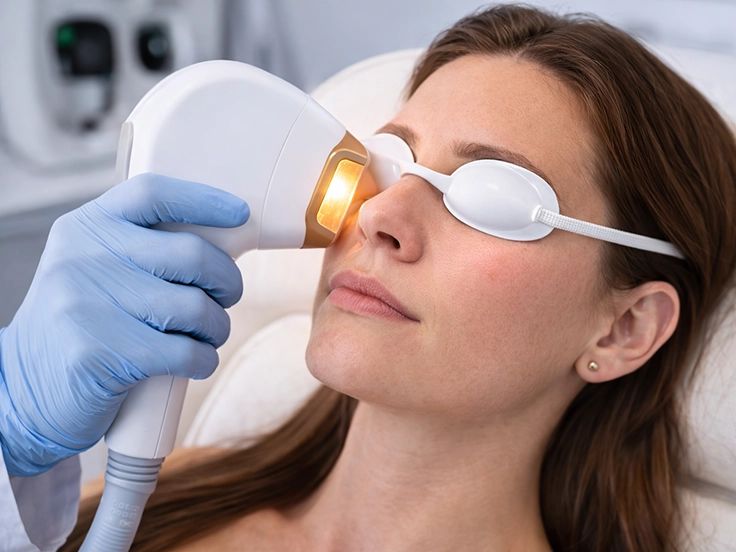
Who it’s for: People with evaporative dry eye, especially when meibomian gland dysfunction (MGD) or eyelid inflammation is a major factor. It has also been shown to be effective in Sjogren’s syndrome.
What it does: Uses high energy pulses of light around the eyelids and face to reduce inflammation and help the oil glands function better.
Why it’s helpful: Targeting inflammation in and around the eyelids promotes healthier oil flow which slows tear evaporation, which often improves comfort and more stable vision.
What to expect during your appointment: The treatment is done in the office and typically takes 30 minutes from start to finish. Numbing eyedrops will be used and protective corneal shields will be placed in the eyes. A series of IPL pulses will be applied to the face and the eyelids. We finish the session with a meibomian gland expression. A series of 4 treatments spaced 3 to 4 weeks apart is required initially, then single maintenance treatments are typically done every 6 to 12 months ongoing.
Low Level Light Therapy (LLLT)
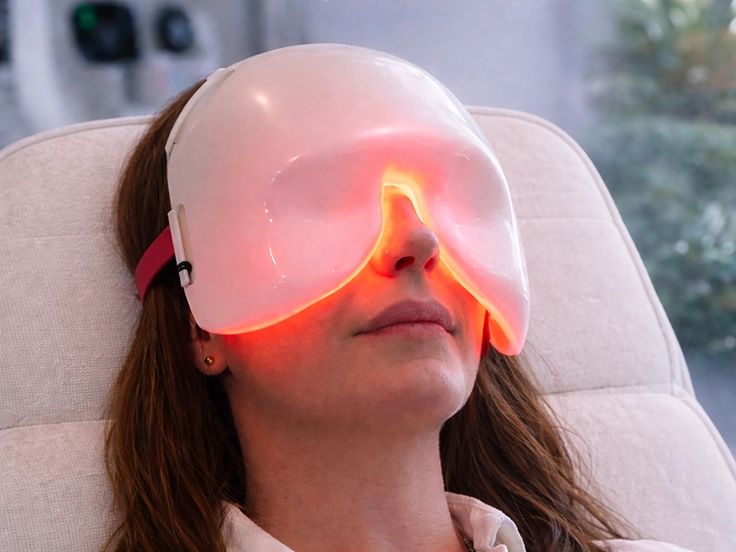
Who it’s for: Patients with dry eye related to MGD who want a gentle, non-invasive option, or who need extra support alongside other treatments.
What it does: Uses low-level LED light to support eyelid and gland health and reduce irritation.
Why it’s helpful: It can help improve comfort by supporting better gland function and a more stable tear film.
What to expect during your appointment: You relax comfortably while the light therapy is applied. Most patients describe it as warm and easy, with little to no downtime.
OptiVize
Who it’s for: Patients with moderate chronic MGD-related dry eye. Many patients have a red line on their upper eyelids indicating Deep Subdermal Blepharitis causing chronic inflammation and blockage of the meibomian glands.
What it does: Targets bacterial biofilm that causes blockage and buildup inside the meibomian glands and at the eyelid margin, often followed by heated expression to improve oil flow.
Why it’s helpful: By addressing gland obstruction at the source, OptiVize can help restore healthier oils in the tear film, reducing evaporation and improving long-term comfort.
What to expect during your appointment: This is an in-office procedure designed to eliminate bacterial biofilm on the eyelids and in the meibomian glands. Each treatment involves a three step process:
- Blephex microblepharoexfoliation (specialized scrubbing of the eyelid margins)
- Vaporization of the biofilm inside the meibomian glands with OptiVize (special contact lens that runs an electrical current through the eyelids)
- Heated expression of the meibomian glands with heated vibratory forceps.
The treatment typically takes 30 minutes. OptiVize is designed to be initially repeated four times on a monthly basis, then ongoing maintenance treatments are spaced out up to 6 months apart, similar to a dental cleaning schedule.
Dry Eye: What Patients Ask Most
Dry eye is common, and symptoms can vary from day to day. These FAQs cover the most common questions we hear from patients.
?When the surface of your eye gets irritated, it can trigger reflex tearing - your eyes “flood” as a response to dryness. The problem is those tears are often too watery and do not stay on the eye long enough to keep it comfortable.
?Wind and dry air make your tears evaporate faster. If your tear film is already unstable (often from MGD), these conditions can quickly lead to burning, watering, and blurry vision.
?Dry eye symptoms are often asymmetric. One eye may have more gland blockage, a slightly different eyelid shape, or more exposure from blinking patterns - so symptoms can feel stronger on one side.
?Outdoor wind, cold, and sun can irritate the eye and trigger reflex tearing, but those tears may not contain enough of the oil layer needed to stay on the eye. So you can have watery eyes and still feel dry.
?MGD (meibomian gland dysfunction) is common and often feels like burning, grittiness, watering, or fluctuating vision that is worse with screens or dry air. The only way to know for sure is an exam where we look at your eyelids and glands and check the quality of the oils in your tear film.
?If you have been consistent for a few weeks and still have symptoms, or if relief is only short-lived, it may be time to add prescription support or consider in-office treatments. Also consider stepping up sooner if dry eye is affecting your vision, contact lens comfort, or daily activities.
?Dry eye can flare based on triggers like screen time, sleep, stress, allergies, weather, heating/AC, and contact lens use. Because the tear film is sensitive, small changes in your routine or environment can cause big swings in symptoms.
?Many drops add temporary moisture, but they do not always fix the underlying issue - especially if tears evaporate quickly due to MGD. In those cases, you may need a different type of drop, better eyelid routine, prescription treatment, or an in-office option.
?Dry eye is often a chronic condition that needs ongoing maintenance. Symptoms can return if the tear film becomes unstable again - for example, if gland blockage builds back up, routines stop, or triggers (screens, dry air, allergies) increase.
?Some people feel improvement within days, especially with the right drops and consistent eyelid care. For many, more noticeable and stable relief takes a few weeks, and advanced treatments like IPL, LLLT, or OptiVize may be recommended as part of a plan over time. The timeline depends on what’s causing your dry eye and how severe it is.
Ready for Dry Eye Relief?
Dry eye can be frustrating, but the right plan can make a real difference. Schedule a dry eye evaluation to find out what’s causing your symptoms and which treatments are most likely to help.
Schedule a Dry Eye Evaluation